Point-of-Care Perspectives from PatientPoint

Video: Must have features in engagement tech for eye care patients
Here are the 3 features you should look for in patient engagement technology to help patients become active partners in eye care decisions.

What are digital healthcare devices for employee engagement?
Learn the ins and outs of digital healthcare devices for employee engagement and why every practice should have one.

How does engagement tech effectively educate patients in the waiting room?
If you don’t have patient engagement technology in the waiting room, you’re missing out an opportunity to educate and prepare patients for their appointment. Here’s why.

How to identify SDOH using technology in your practice
Learn how your practice can screen for and address social determinants of health using patient engagement technology.

What is patient engagement technology?
Over the years, healthcare practices have adopted the conveniences of the consumer experience—including online forms and appointment scheduling. Innovations in technology have made these modern

Close the deal with in-office marketing
The right in-office marketing strategy can provide value to you and your patients. Here’s how to effectively do so using healthcare signage.
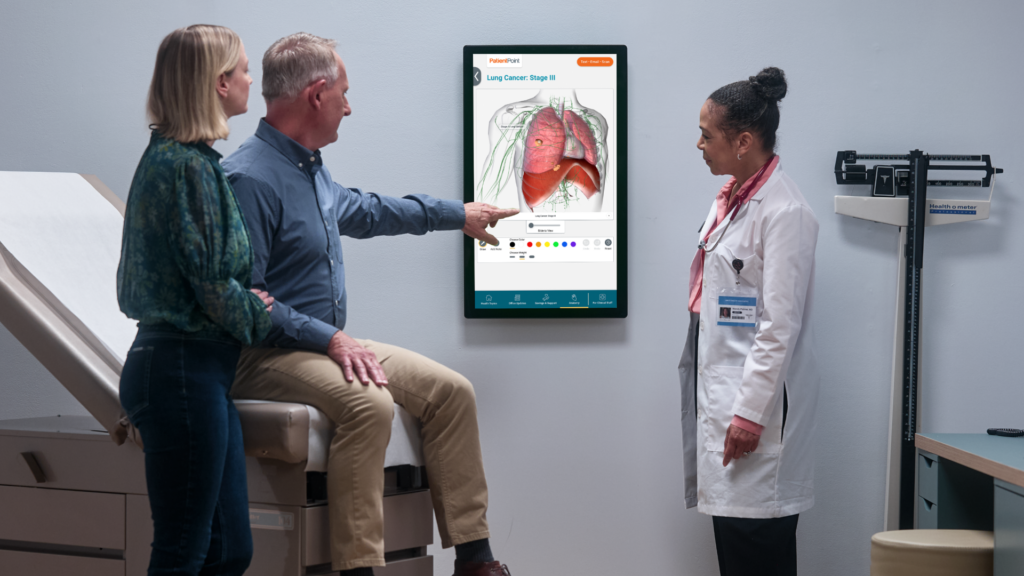
How exam room devices affect patients
Imagine an exam room where patients actively participate in their health journey and ask questions about their condition and treatment—a room where complex medical concepts
